North Bethesda
Expert periodontal, laser, and implant solutions tailored to restore oral health and confidence.

What Makes Us Unique
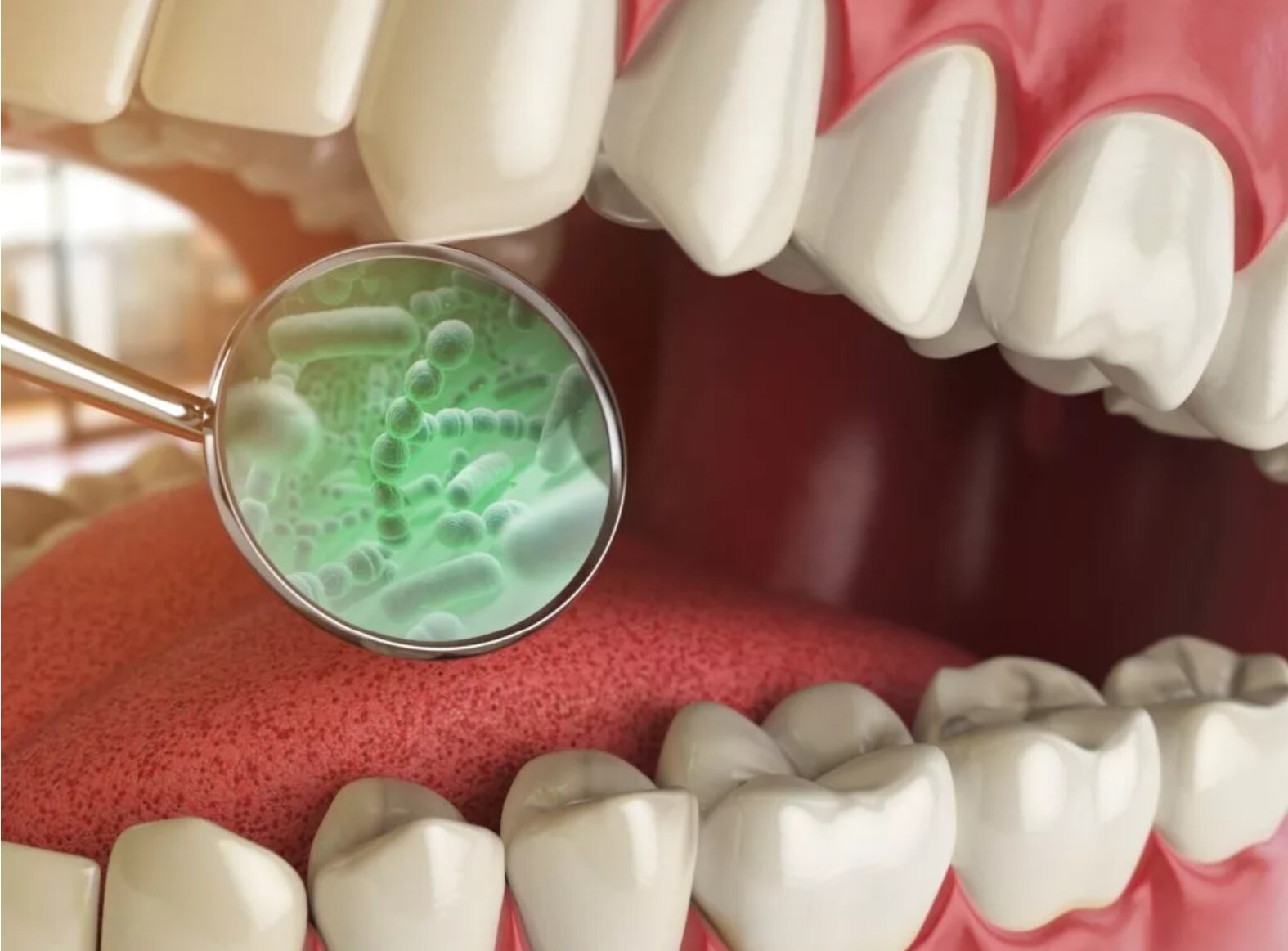
Salivary Microbial DNA Testing and Genetic Susceptibility Testing
Our care goes beyond the surface. Through Salivary Microbial DNA testing, we identify the specific bacteria contributing to gum disease, allowing for customized, targeted treatment plans. In addition, our integrative approach includes IV therapies to enhance healing, reduce inflammation, and support recovery from the inside out.
IV therapy
IV therapy extends far beyond sedation. It serves as a versatile route for delivering a wide range of treatments, including anti-inflammatory medications, antibiotics, and analgesics—allowing for precise, efficient, and targeted patient care.
Laser therapy
Laser therapy is not limited to surgical procedures. It also plays a valuable role in a variety of non-surgical applications, such as photodynamic therapy and laser photo biomodulation, offering therapeutic benefits that support healing, reduce inflammation, and enhance overall treatment outcomes
Problems We Treat
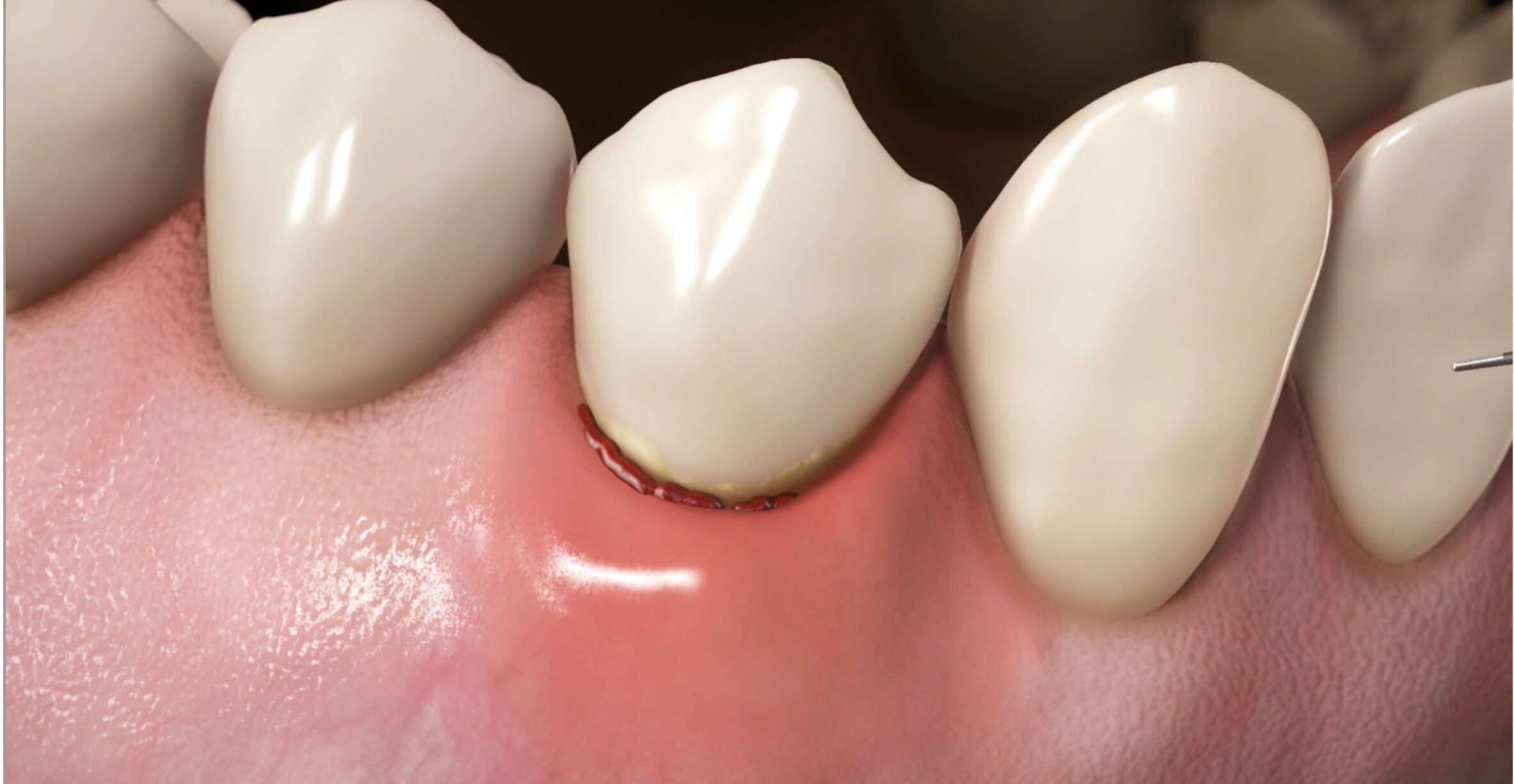
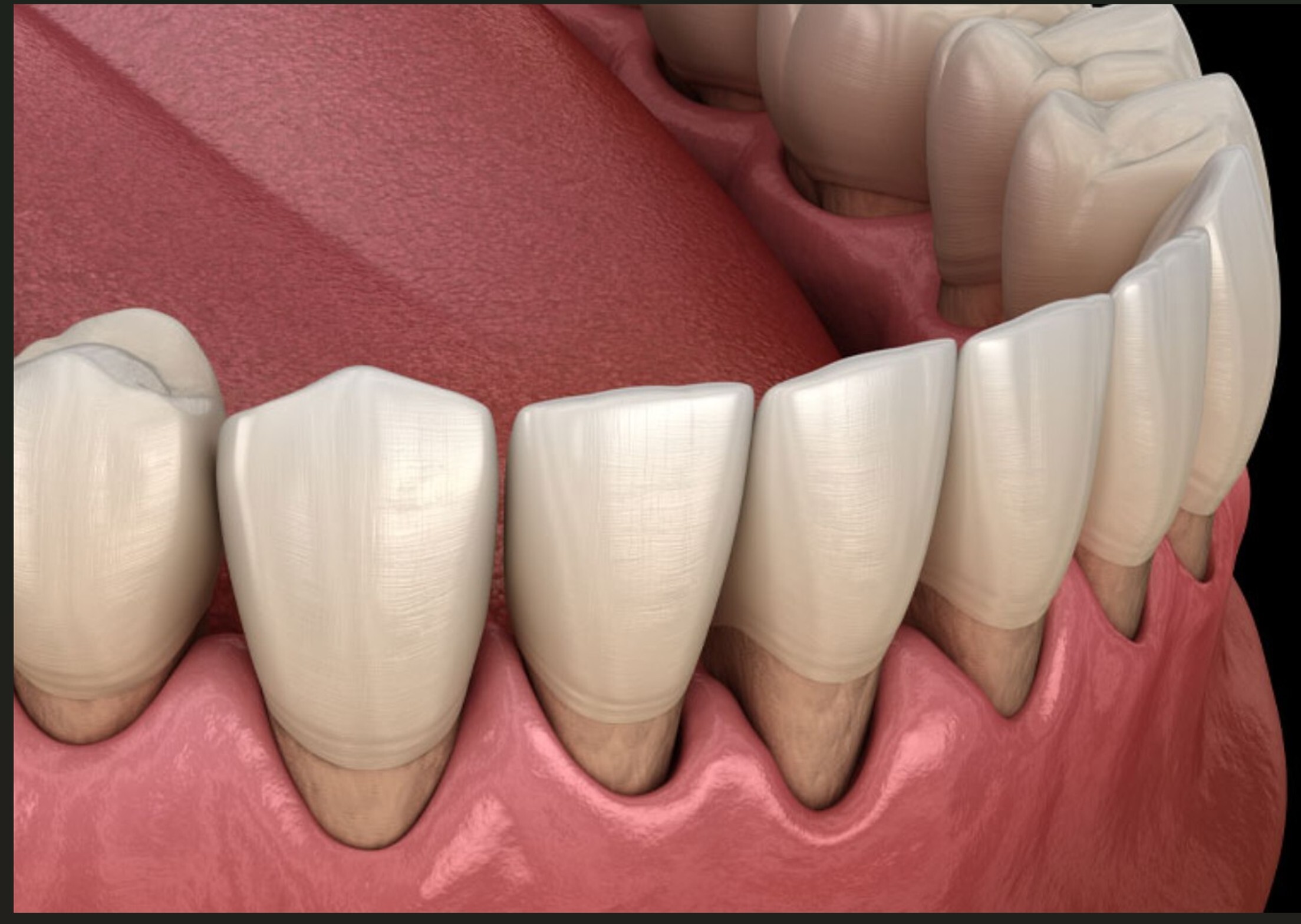
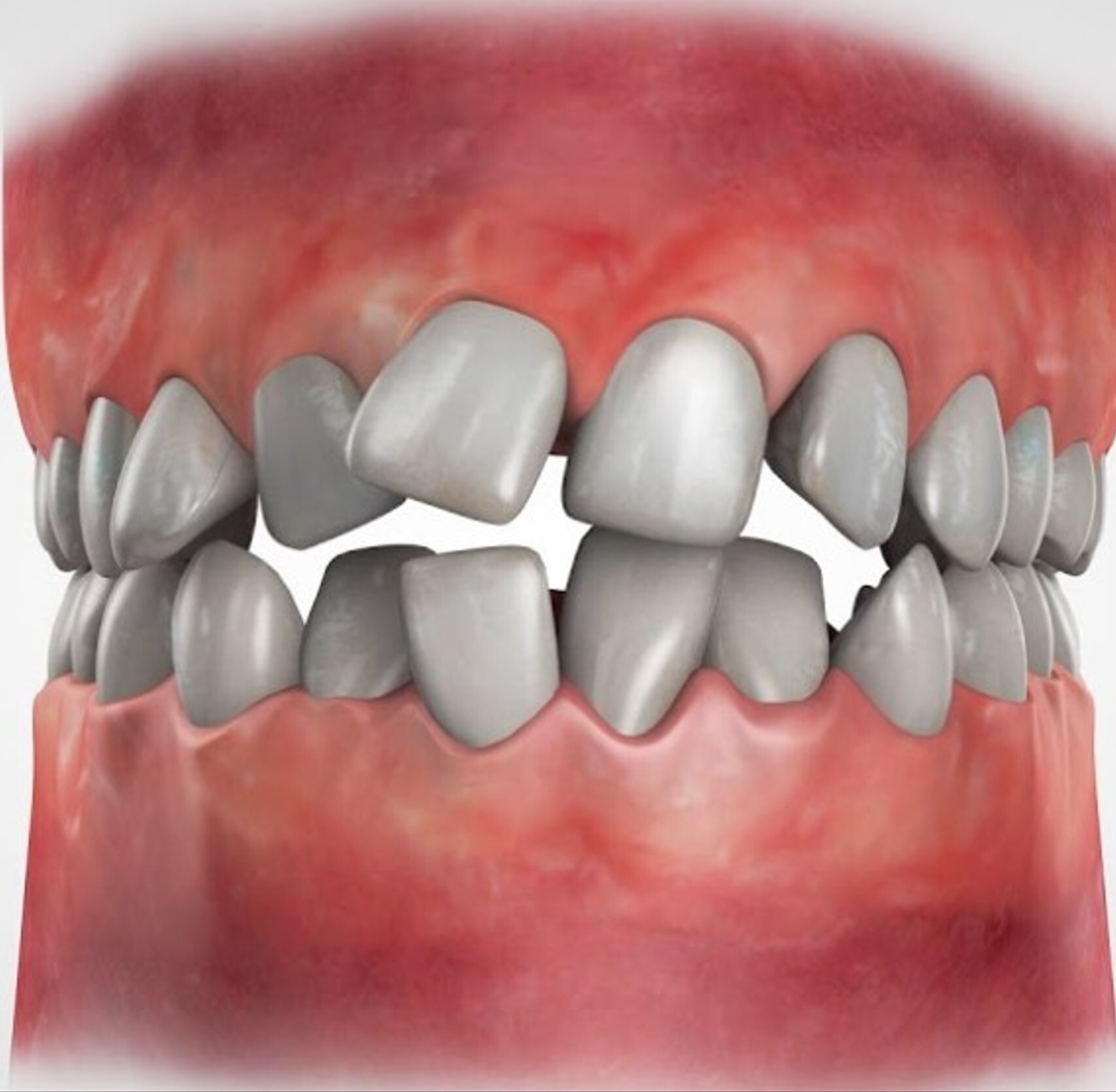
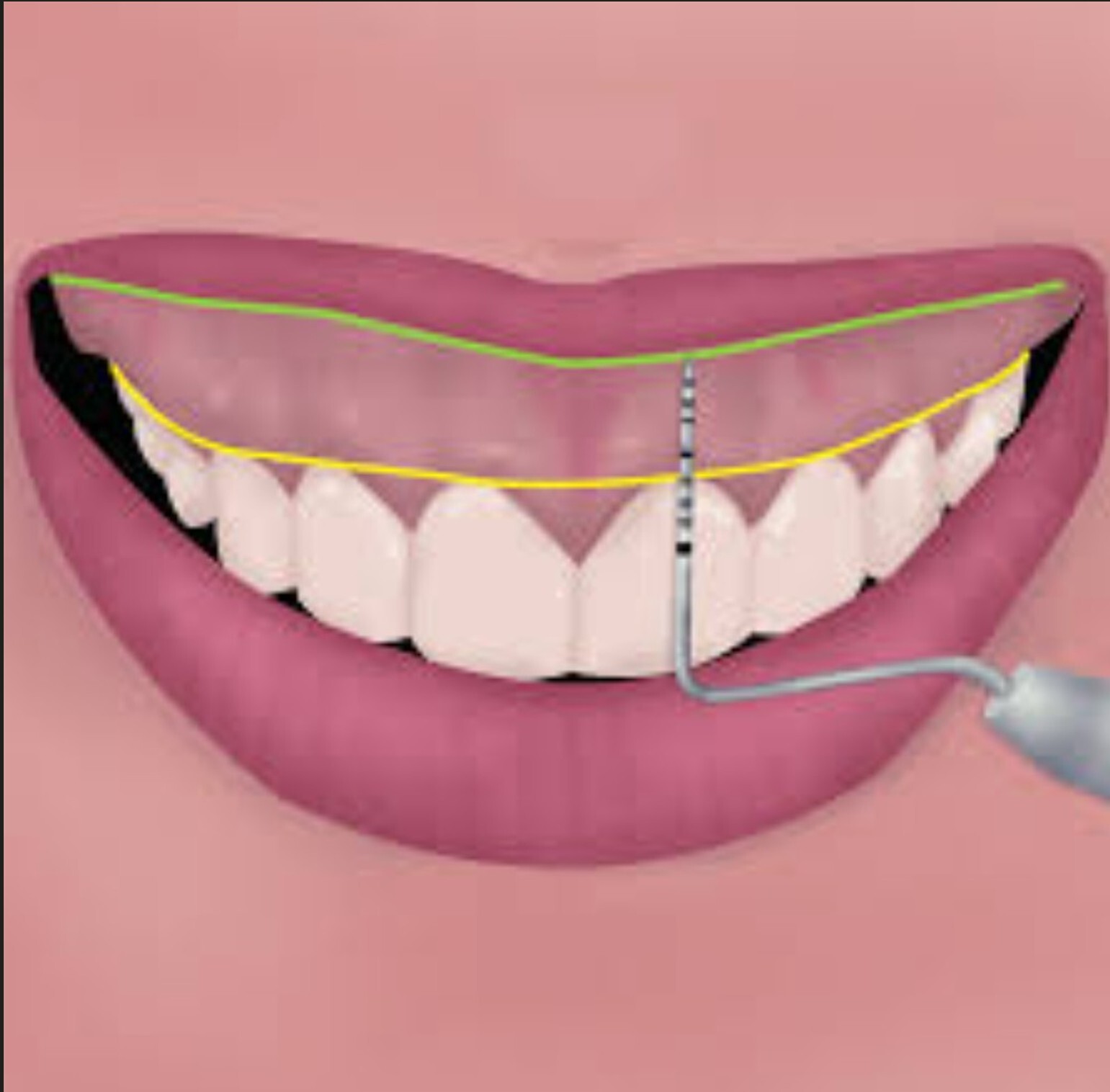
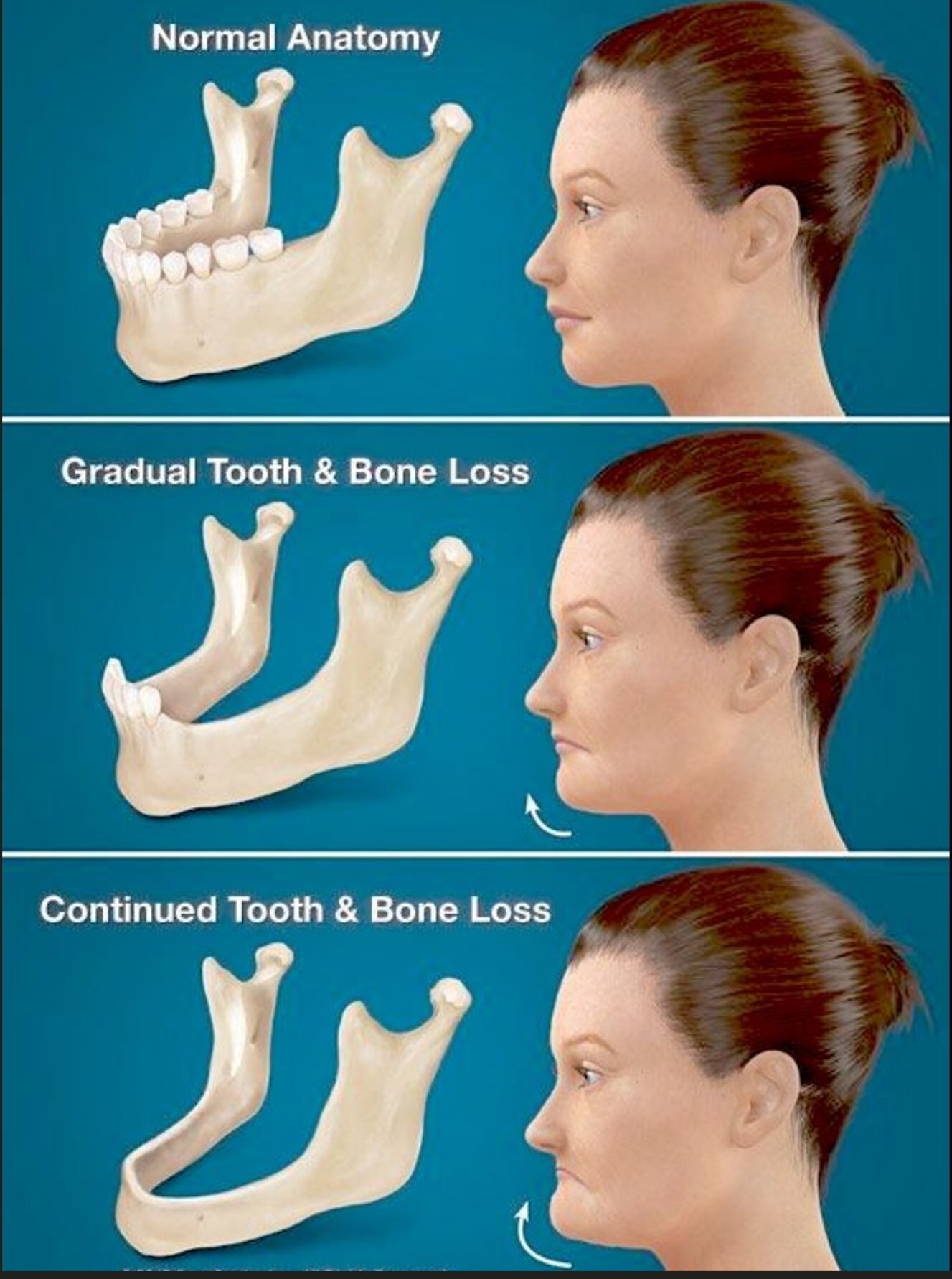
Healing Gum Infections, Receding Gums, and Bleeding Gums in North Bethesda, Potomac, and Rockville
We treat gum disease, bone loss, and oral health concerns using advanced diagnostics and minimally invasive techniques.
If you're experiencing any of these symptoms, don't wait. Early treatment can save your teeth.
Treatments We Offer
Advanced Periodontal and Implant Treatments for Optimal Healing
We combine science, artistry, and regenerative technology to restore oral health and aesthetics.
Explore minimally invasive, biologically driven periodontal care.
Lifelong Learning and Leadership
Our clinical team is actively involved in continuing education, research, and mentorship. We strive to lead by example and stay at the forefront of the profession—so our patients always benefit from the most current and effective techniques available.
Periodontal Services
Our comprehensive periodontal services focus on diagnosing and treating diseases affecting the gums and supporting structures of the teeth. Utilizing advanced tools like advanced biologic diagnostic testing, we precisely identify your genetic susceptibility and specific bacteria’s contributing to gum disease, allowing for targeted, effective treatment plans
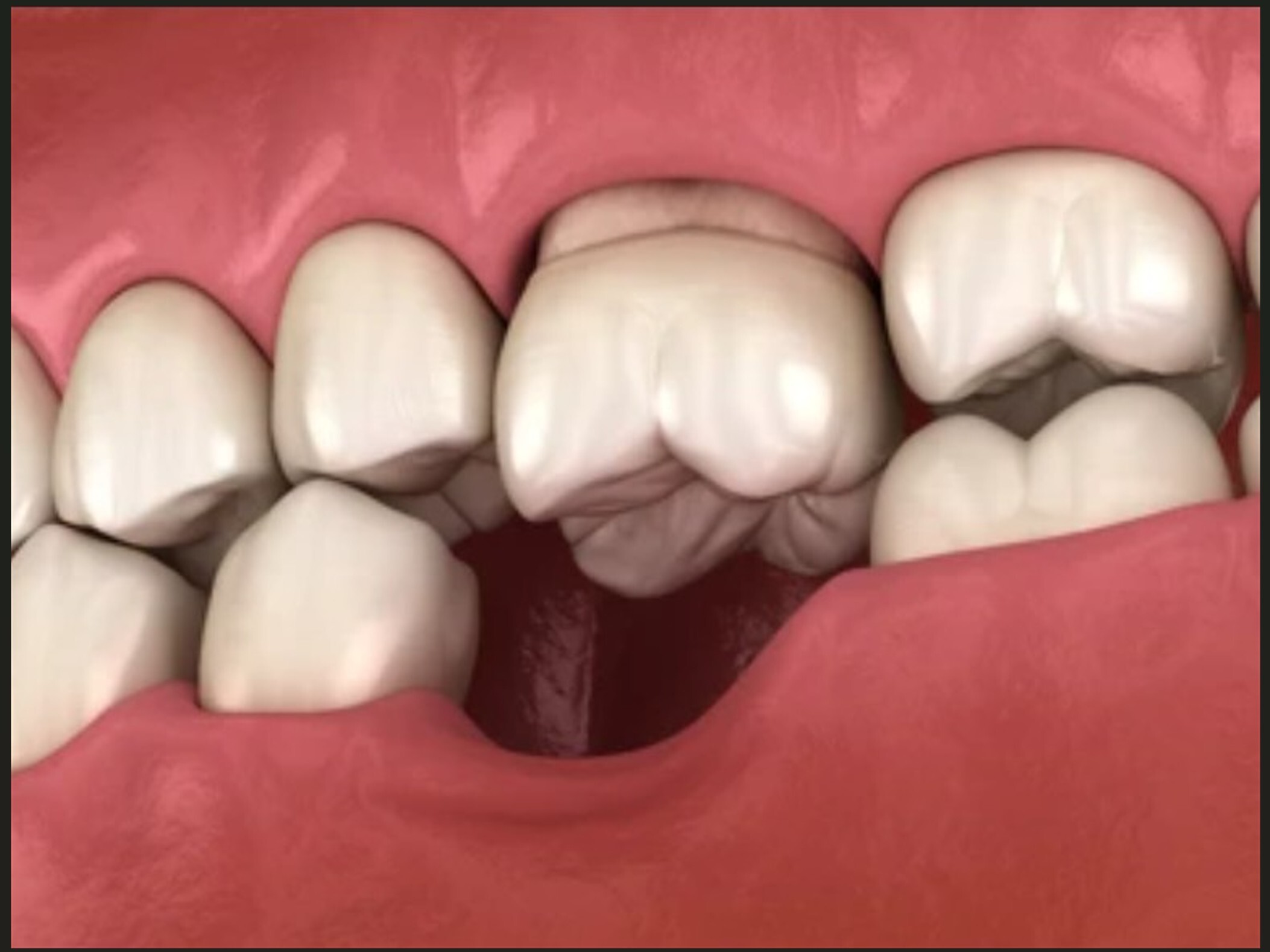
Dental Implants
Dental implants offer one of the most natural and durable solutions for replacing missing teeth—restoring both function and aesthetics without compromising neighboring teeth. Whether you’re missing one tooth or several due to trauma, decay, or gum disease, implants can help you chew, speak, and smile with confidence.
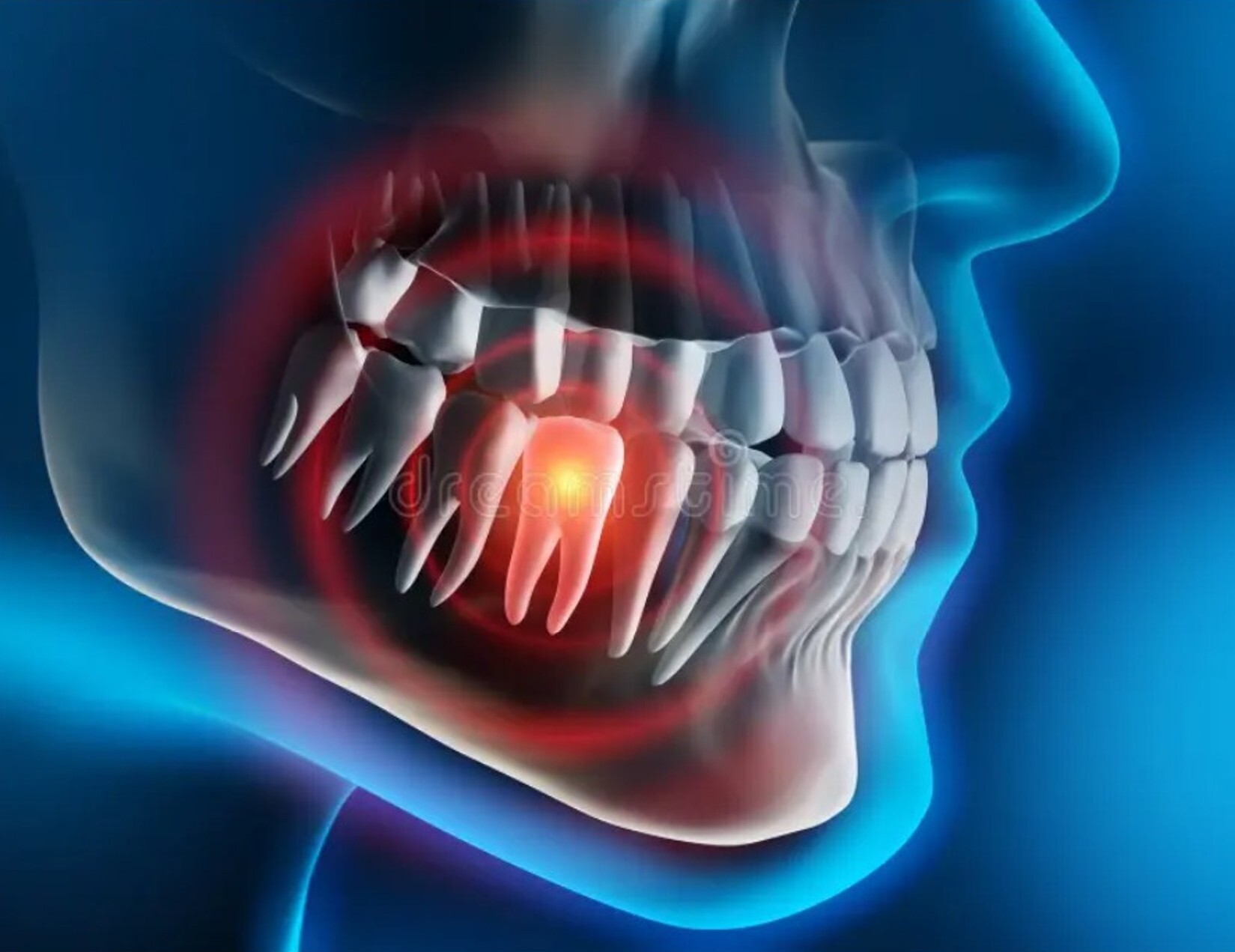
Oral Surgery
When a tooth can no longer be saved due to extensive decay, trauma, or advanced gum disease, extraction may be the best option to protect your overall oral health. At Potomac Periodontics and Implant Center, we perform tooth removals using precise, minimally invasive methods designed to minimize discomfort and support swift recovery
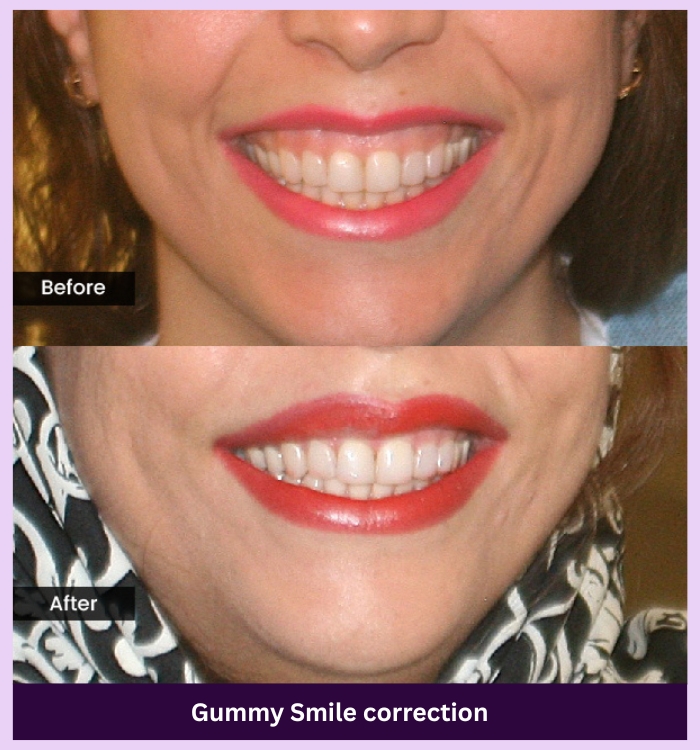
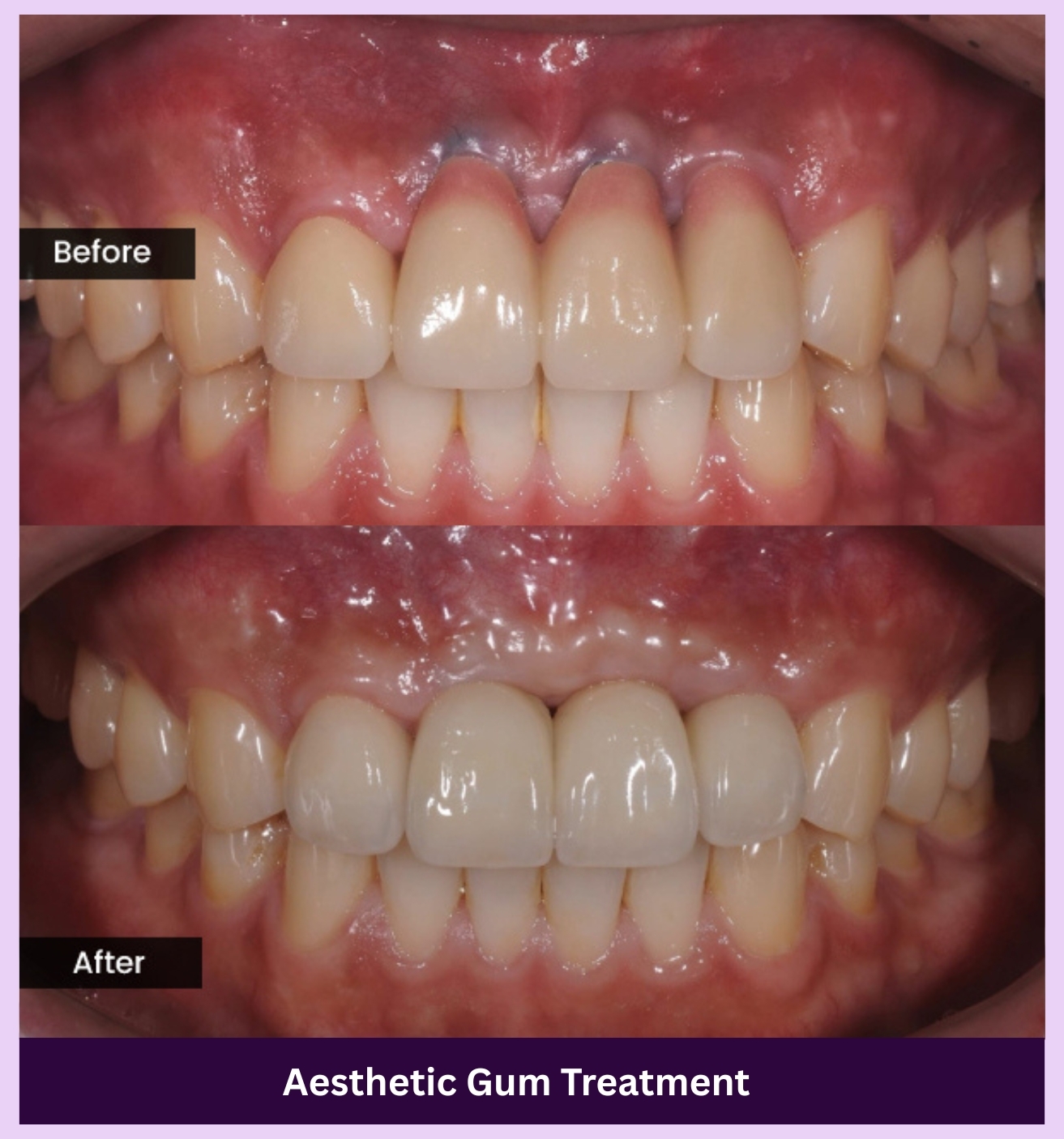
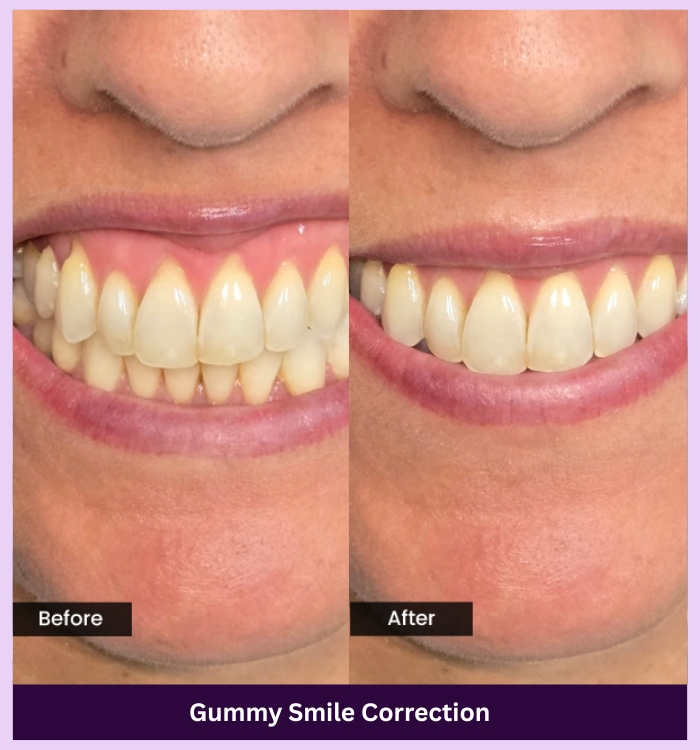
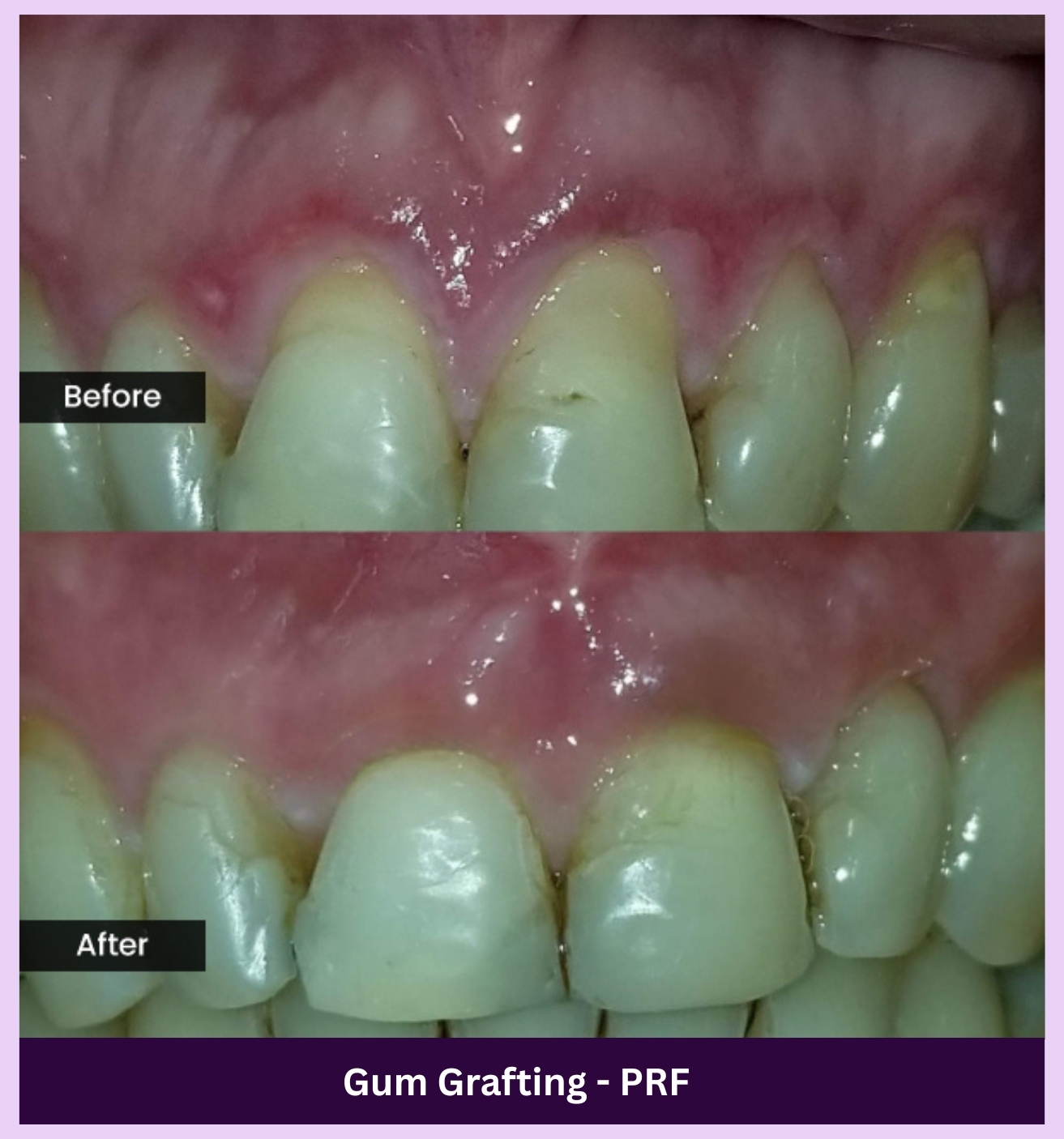
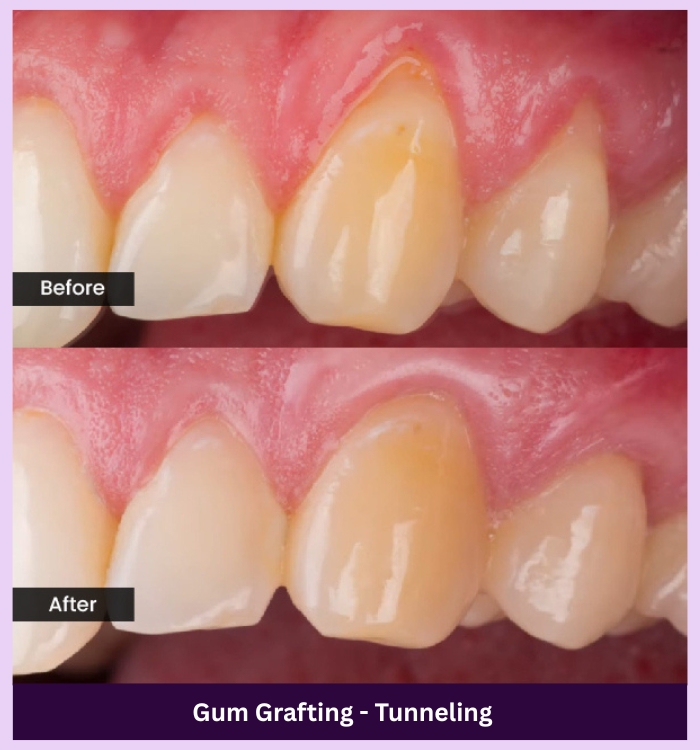
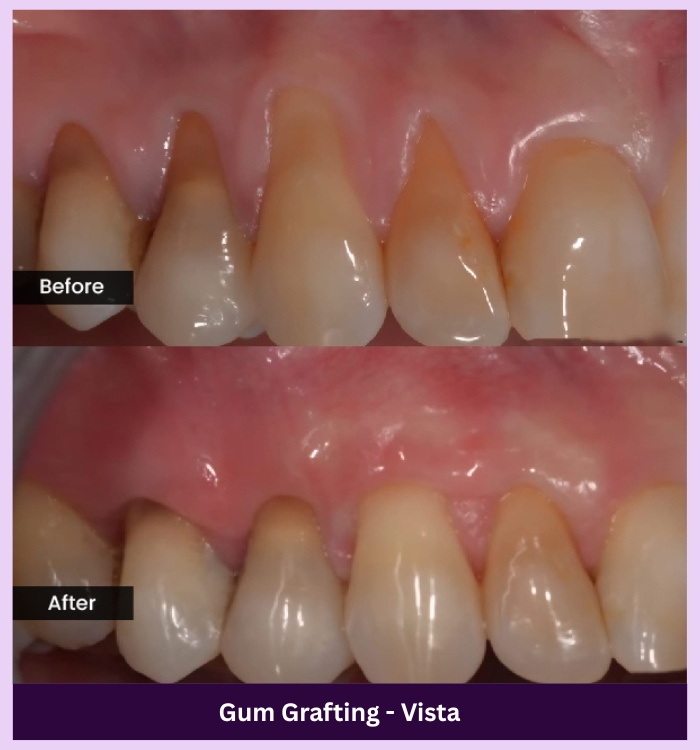
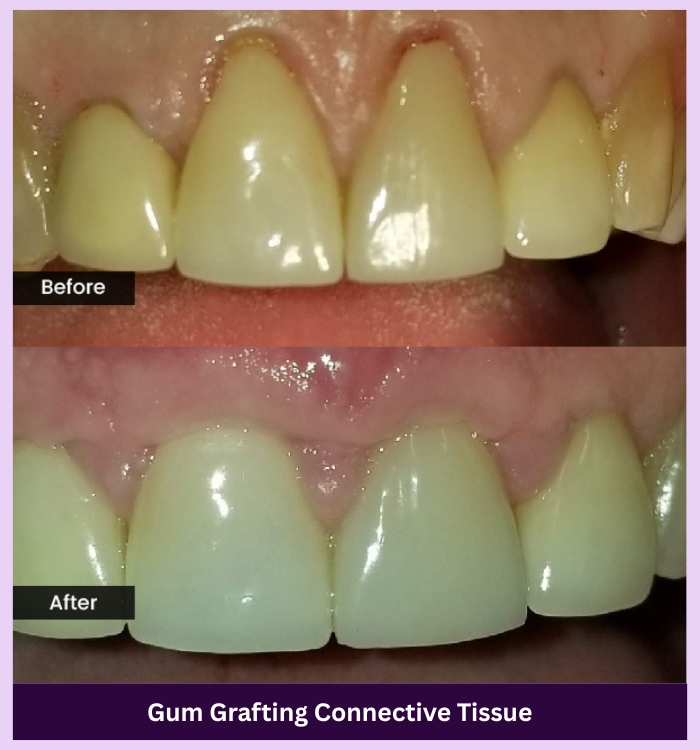
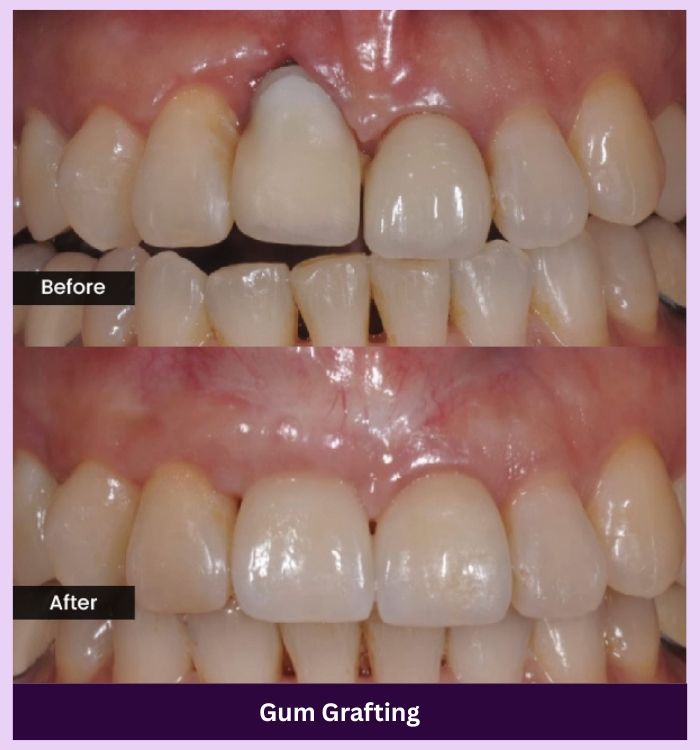
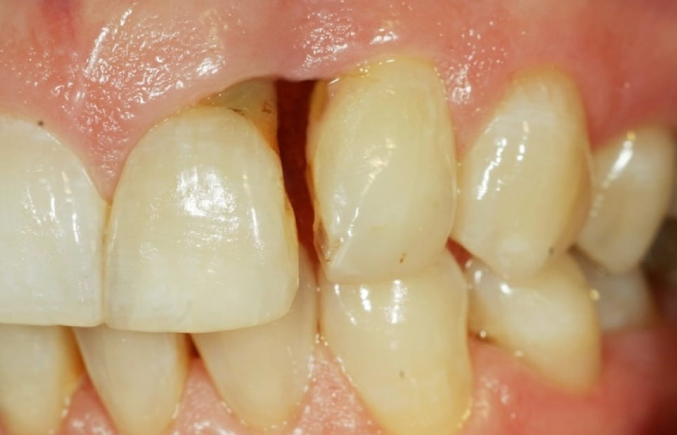
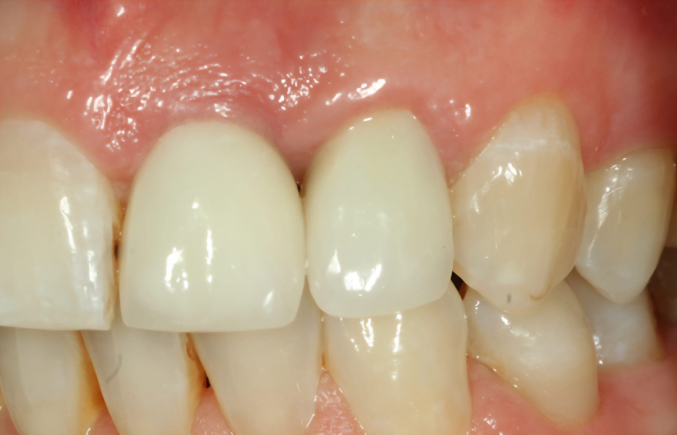
SEE THE DIFFERENCE
Make your smile shine again
Trustindex verifies that the original source of the review is Google. (2 implants & bone grafting) I was nervous about the entire procedure but the Doc erased all my anxiety and the end product is spectacular. His manner and skillset are top-notch!Posted onTrustindex verifies that the original source of the review is Google. I appreciate this Dentist very much. I was in great distress because of pain and infection and he made everything which was hurting me To go away and I will be soon getting two new implants and the infection is all gone plus, he was very kind to me and gentle as the ladies who work in the office assured me, he would be previous to my Getting work done. Sincerely, K. Leanne Mikesell.Posted onTrustindex verifies that the original source of the review is Google. I had a broken tooth. All doctors wanted the tooth extracted. Dr. Vanities saved my tooth by doing a crown lengthening. Thank youPosted onTrustindex verifies that the original source of the review is Google. Exceptional care and precision in gum grafting and Implant surgery! If you’re looking for expert Implant placement with advanced technology, Dr. Vaziri is the one! Thank you Doctor!!!Posted onTrustindex verifies that the original source of the review is Google. I had been struggling with sensitivity in my lower teeth for months and saw multiple dentists who couldn’t pinpoint the exact problem. Dr. Vaziri was the only one who took the time to carefully evaluate everything and helped me identify the exact tooth causing the issue. He also performed an extraction and placed an immediate implant with such skill and care that I felt completely at ease throughout the process. I’m so grateful for his expertise and highly recommend him to anyone looking for a knowledgeable and compassionate periodontist.Posted onTrustindex verifies that the original source of the review is Google. I had a tooth decay. Doctor extracted my decayed tooth from bone grafting to implant placement doctor vaziri provided the best care.Posted onTrustindex verifies that the original source of the review is Google. I was nervous about getting implants but Dr Vaziri made it comfortable and stress free.Posted onTrustindex verifies that the original source of the review is Google. Dr. Vaziri is a master of dental implants—painless procedure and amazing results!Posted onTrustindex verifies that the original source of the review is Google. Dr Vaziri, is incredibly skilled compassionate, and transformed my smile- highly recommend. Very happyPosted onTrustindex verifies that the original source of the review is Google. Dr. Vaziri has been great in saving my teeth and only giving me the implants I needed (unlike another periodontist who wanted to just pull all my teeth). It’s been as great an experience as any dental work can be!
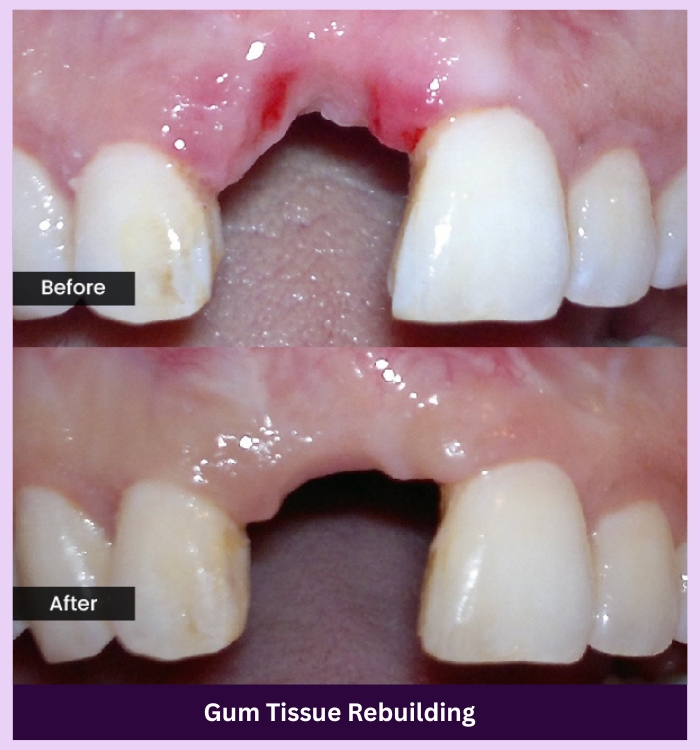
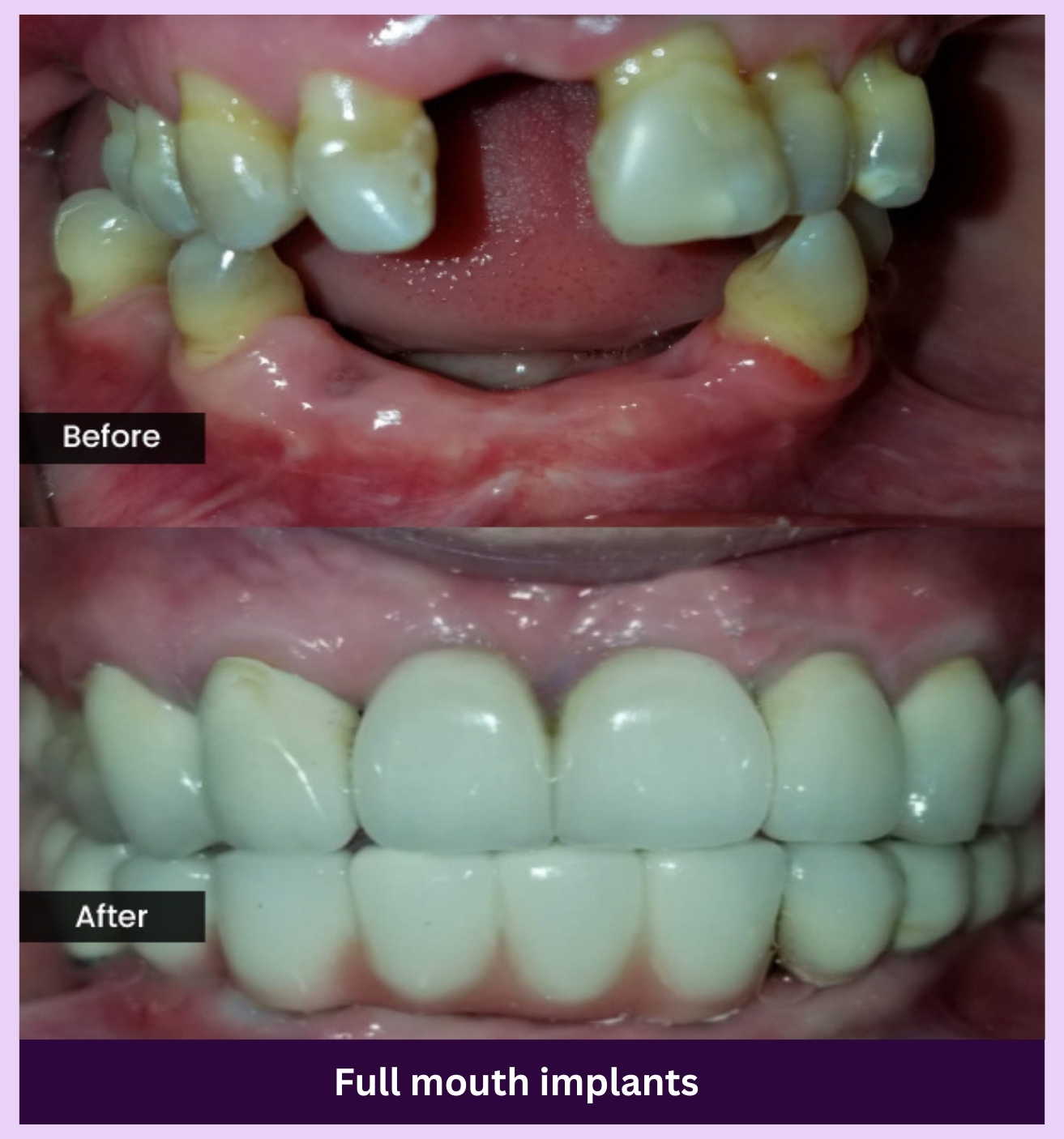
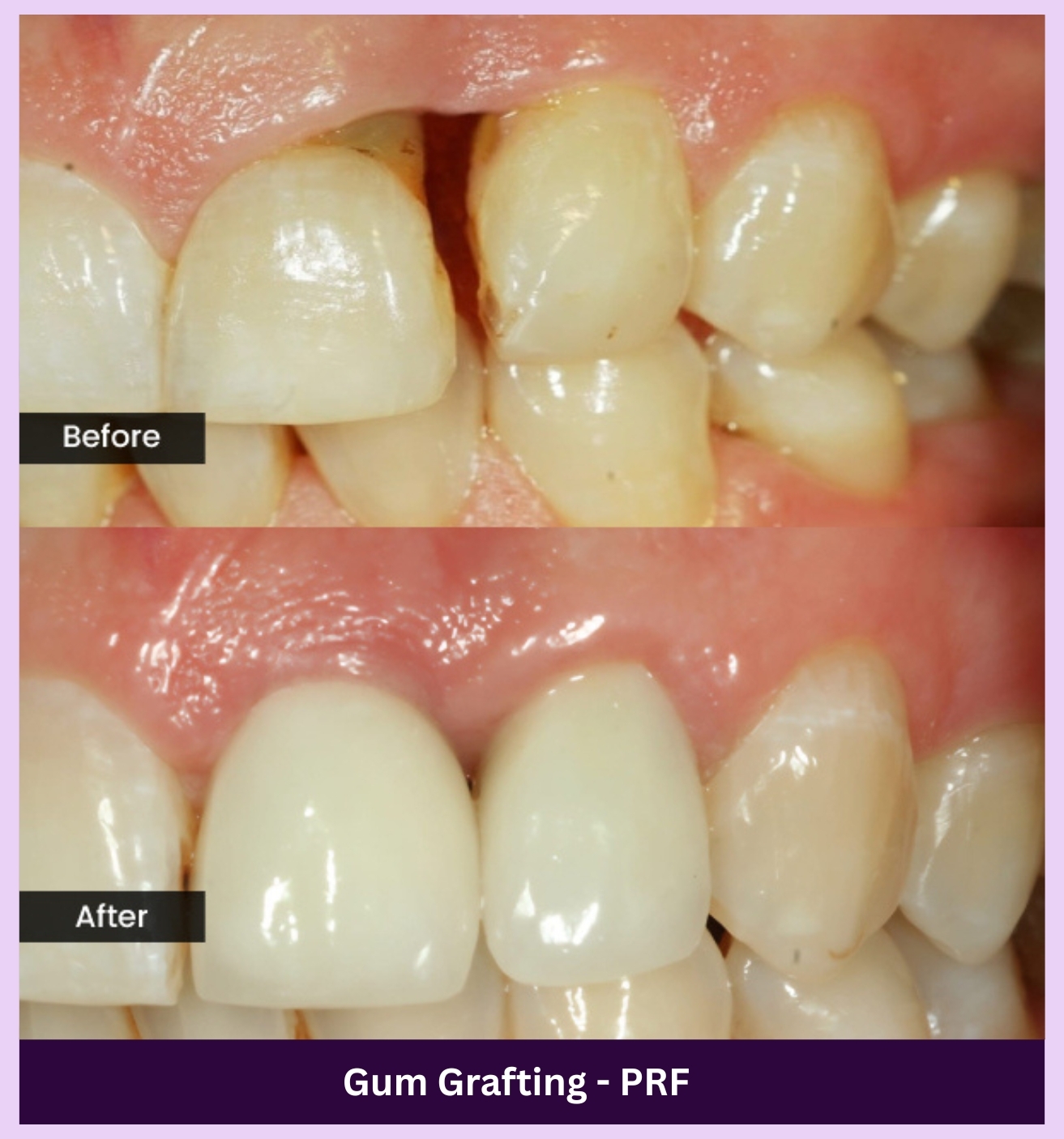
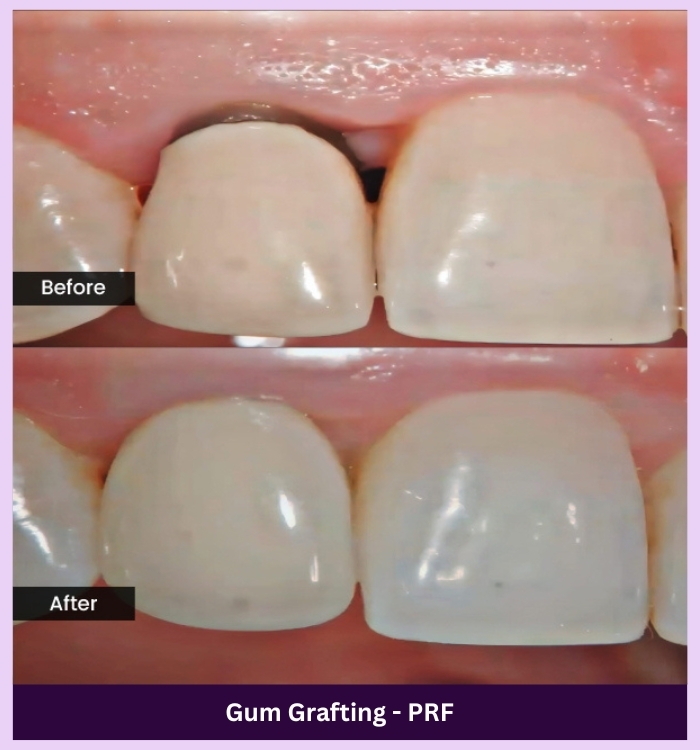
OUR GALLERY